Benefits of Fascia Massage: Who Should Try It
May 10, 2026
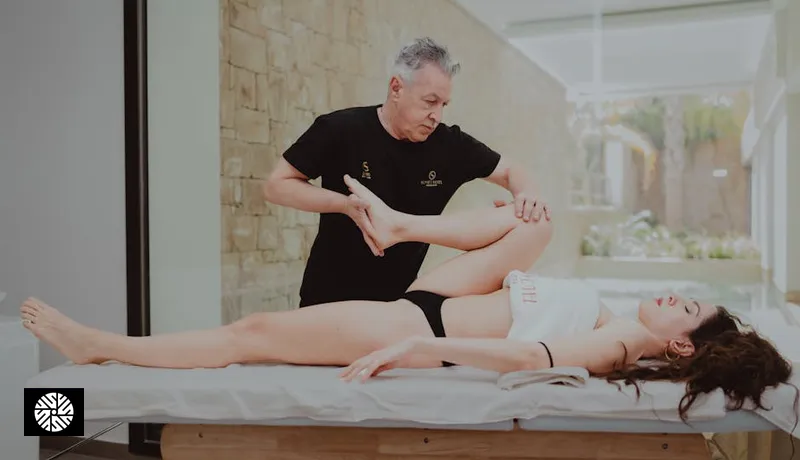
Fascia massage gets talked about as a universal cure for stiffness, soreness, and posture problems. The reality is more specific. Certain people, with certain dysfunctions, get genuinely meaningful relief from skilled fascial work — sometimes results that they could not get from conventional massage, stretching, or even physical therapy alone. Other people see modest improvements. And a few should not be receiving fascia work at all, at least not right now.
This article walks through who actually benefits, which specific conditions respond well, how to think about timing and frequency, and where the evidence is strong versus where it is thin. It is the practical follow-up to our anatomy primer on fascia — instead of explaining what fascia is, we are answering the question patients actually ask: is this for me?
Beneficiary profiles — who genuinely benefits
Fascia work is most useful for people whose problem is not primarily muscular or skeletal, but connective-tissue based — restriction, adhesion, densification, scar tissue. Six broad groups consistently report meaningful outcomes:
- Chronic pain sufferers — low back pain, neck pain, cervicogenic headache, plantar fasciitis, IT band syndrome, myofascial pain syndrome.
- Post-surgical patients — scar tissue mobilization after c-section, mastectomy, abdominal surgery, knee or hip replacement.
- Athletes — runners, cyclists, lifters, climbers with sport-specific tightness in the IT band, hamstrings, calves, shoulder capsule, or thoracolumbar fascia.
- Office workers — "tech neck," forward head posture, kyphotic shoulders, hip flexor tightness from prolonged sitting.
- Aging adults — age-related fascial densification, reduced glide between tissue layers, and the stiffness that accompanies sarcopenia.
- Pregnant and postpartum people — gentle work to support diastasis recti recovery, pelvic floor restoration, and posterior chain rebalancing.
| Beneficiary profile | Primary concerns | Suggested frequency |
|---|---|---|
| Chronic pain sufferer | Low back, neck, headache, plantar fasciitis | Weekly for 4-6 weeks, then biweekly |
| Post-surgical (cleared by surgeon) | Scar mobilization, adhesion prevention | Every 1-2 weeks for 8-12 weeks |
| Athlete (in season) | IT band, hamstrings, shoulder, calves | Every 2-3 weeks, recovery-focused |
| Office worker | Tech neck, forward head, hip flexor tightness | Monthly maintenance, more if symptomatic |
| Aging adult (60+) | Fascial densification, general mobility | Every 3-4 weeks, gentler pressure |
| Postpartum (6+ weeks) | Diastasis recti, pelvic floor, posture | Every 2 weeks for first 3 months |
| Healthy adult (maintenance) | General mobility, stress, sleep quality | Once a month or post-trip |
The frequencies above are starting points, not prescriptions. A good practitioner will adjust based on how your tissue responds and how durable the changes feel between sessions.
Chronic pain — low back, neck, headache, plantar fasciitis
If you have had pain in the same region for more than three months, and conventional approaches (NSAIDs, basic physical therapy, stretching) have plateaued, fascia work is one of the more reasonable next steps to try. The conditions with the most clinical track record are:
Chronic low back pain. The thoracolumbar fascia is a dense, multi-layered sheet that connects the lats, glutes, and lower back into a single functional unit. When it densifies or develops adhesions, normal load-sharing breaks down and the muscles around it have to compensate — which is what most people feel as "back tightness." A typical protocol involves direct work on the thoracolumbar fascia, glute medius, and quadratus lumborum, with attention to the hip flexors as a counterbalance.
Neck pain and cervicogenic headache. Many headaches that get labeled "tension headaches" are actually driven by restrictions in the suboccipital region and the deep cervical fascia. Releasing these can reduce headache frequency and intensity within 2-4 sessions for patients whose pain pattern matches. The work usually pairs cervical fascia release with thoracic outlet and upper trapezius.
Plantar fasciitis. This is one of the clearest indications for fascia work. The plantar fascia rarely operates in isolation — the calf, achilles, and posterior chain pull on it constantly. A good plantar fasciitis protocol works the foot itself, then the gastrocnemius and soleus, then often the hamstrings. Single-session relief is common; durable change usually takes 4-6 sessions plus eccentric calf loading at home.
IT band syndrome. The IT band is not really a muscle and does not "release" the way people imagine. What does change is the glute medius, the lateral quad (vastus lateralis), and the tensor fascia latae upstream. Working those structures — not just rolling on the IT band itself — is what reduces lateral knee pain.
Post-surgical recovery — scar mobilization
Scar tissue is essentially disorganized fascia. Left alone, it can adhere to surrounding structures and create restriction far from the original incision — sometimes years after the surgery. Manual scar mobilization, started at the right time, helps the new tissue lay down in a more functional pattern.
Three contexts where this matters most:
- C-section recovery. Once the wound is fully healed (typically 6-8 weeks, with surgeon clearance), gentle work around the scar can reduce pulling sensations, improve abdominal function, and address the low back pain that often follows c-section recovery. Many people are never told this is an option.
- Post-mastectomy. Lymphatic flow, shoulder mobility, and chest wall flexibility are all affected by mastectomy and reconstruction scars. Specialized post-mastectomy bodywork — done by practitioners with oncology massage training — can restore range of motion and reduce cording.
- Joint replacement (knee, hip). The incision scar from a knee or hip replacement can adhere to deeper tissue layers, limiting the recovery of full range of motion. Fascia work as an adjunct to standard post-op physical therapy often improves outcomes, particularly between weeks 6 and 16.
The non-negotiable rule: do not start manual work on a surgical area until your surgeon has confirmed the wound is fully healed. Typically that is 6-8 weeks minimum for soft-tissue surgeries, longer for orthopedic procedures.
Athletes — IT band, hamstrings, post-workout
For athletes, fascia work is best framed as a recovery tool, not a performance tool. The evidence that it directly improves performance is thin. The evidence that it helps recovery, reduces post-session soreness, and addresses sport-specific tightness is stronger.
Runners. The classic running problem areas — plantar fascia, calves, hamstrings, glute medius, IT band — all benefit from regular fascial work. Most serious runners find a 60-90 minute session every 2-3 weeks is enough to keep tissue mobile, with more frequent visits during high-volume training blocks.
Cyclists. Hip flexors, anterior thigh, and thoracic spine are the priority. Cycling locks the body into a flexed posture for hours, and fascia work targeting the anterior chain helps undo it.
Lifters. The shoulder capsule, lats, and thoracolumbar fascia take the most load. Mobility-focused fascia work in the off-season or during deload weeks tends to produce better results than chasing it during heavy training.
Timing matters: same-day or pre-event fascia work is generally a bad idea. The temporary mobility increase can affect proprioception and tendon stiffness in ways that don't help — and sometimes hurt — competition performance. Better to schedule fascia work 2-4 days before a key event, or in the recovery window 24-72 hours after.
Office workers — tech neck, forward head, kyphosis
Eight hours a day at a screen, with the head 2-3 inches forward of neutral, loads the cervical and upper thoracic fascia in a way that human anatomy never evolved to handle. The result is the familiar pattern: forward head, rounded shoulders, kyphotic upper back, tight pectorals, weak deep neck flexors.
Fascia work for postural issues focuses on what is short and tight, not what is weak. The short-tight structures are usually:
- Suboccipital muscles (base of skull)
- Anterior cervical fascia (front of neck)
- Pectoralis major and minor (chest)
- Upper trapezius and levator scapulae
- Thoracolumbar fascia (lower back, from prolonged sitting)
- Hip flexors and rectus femoris
Releasing these structures gives the postural correction exercises (deep neck flexor work, scapular retraction, hip extension drills) a chance to actually take hold. Without releasing the restrictions first, "fix your posture" exercises tend to fight against tight tissue and produce only temporary gains.
Aging adults — fascial densification
Fascia changes with age. The collagen fibers become more cross-linked, the hyaluronic acid that allows tissue layers to glide past each other becomes less hydrated, and movement variety drops — which compounds the stiffness. This is independent of muscle loss (sarcopenia), although the two often happen together.
For adults over 60, fascia work serves a slightly different purpose than for younger patients. The goal is less about resolving a specific dysfunction and more about preserving the ability to move easily through daily life. Lighter pressure, longer holds, and more attention to hydration before and after a session all matter more in this group.
A reasonable starting cadence is every 3-4 weeks. Aging adults who maintain a regular fascia-work practice frequently report better balance, easier mornings (less stiffness on waking), and improved sleep — all of which compound into healthier aging.
Pregnancy and postpartum considerations
During pregnancy, fascia work should be gentle, done by a practitioner with prenatal training, and focused on relief — not deep restructuring. Hormonal changes (relaxin) already increase tissue laxity; aggressive fascia work can destabilize joints that are already loose. Side-lying positioning is standard after the first trimester. Skip deep abdominal work entirely.
Postpartum is where fascia work earns its keep. Once cleared by an OB or midwife (typically 6 weeks for vaginal delivery, 8+ weeks for c-section), gentle fascial work can address:
- Diastasis recti. The connective tissue between the rectus abdominis muscles often needs help reorganizing. Fascia work, paired with appropriate core rehab, supports better closure.
- Pelvic floor support. The fascial network connecting the pelvic floor, abdomen, and diaphragm often needs unwinding after pregnancy and delivery.
- Postural restoration. Carrying a baby in front for nine months — and then in arms for years — creates predictable patterns in the upper back, neck, and shoulders.
Postpartum fascia work pairs especially well with pelvic floor physical therapy. The two address different but overlapping tissues, and most pelvic floor PTs will gladly coordinate with a bodyworker.
Contraindications — when to avoid
Fascia work is generally safe, but there are real contraindications where the risks outweigh any potential benefit. Be honest with your practitioner about your medical history.
| Contraindication | Why it matters |
|---|---|
| Acute injury (sprain, strain, fracture) | Inflammation is still active; manipulation can worsen tissue damage. Wait until acute phase resolves. |
| Recent surgery (under 6 weeks) | Wound healing not complete; risk of disrupting sutures or new tissue formation. |
| Deep vein thrombosis (DVT) — suspected or confirmed | Risk of dislodging a clot. Absolute contraindication. |
| Severe osteoporosis | Risk of fracture from deep pressure. Lighter techniques may still be appropriate — discuss with both doctor and therapist. |
| Active infection (skin, systemic) | Risk of spreading infection or worsening symptoms. Wait for full resolution. |
| Bleeding disorders or anticoagulant therapy | Increased bruising risk; deep pressure may need to be modified or avoided. |
| Recent chemotherapy or radiation | Tissue fragility and immune compromise. Only practitioners with oncology massage training, with oncologist clearance. |
| Open wounds or active skin conditions | Avoid the affected area entirely until healed. |
| Uncontrolled hypertension or cardiovascular disease | Get medical clearance first. Modified, gentler approaches often still possible. |
This list is not exhaustive. Always tell your practitioner about medications, recent procedures, and chronic conditions — even ones that seem unrelated. A skilled therapist would rather adjust technique than risk harm.
Frequency and combining with other recovery
Fascia massage works best as one layer in a recovery stack, not as a standalone fix. The pattern that consistently produces results across all the beneficiary profiles is:
- Active dysfunction (current pain, restricted movement): weekly sessions for 4-6 weeks, then reassess. If meaningful change has not happened by session 6, the diagnosis may be wrong or another modality is needed.
- Maintenance (no current pain, want to stay mobile): every 3-4 weeks is enough for most people.
- Post-trip recovery: a single session after a long flight or stressful travel block, particularly for travelers combining medical care with rest. Two sessions, 3-5 days apart, is even better.
- Pre-event for athletes: schedule 2-4 days before a competition — never same-day.
Combining fascia work with stretching, strength training, and (when relevant) physical therapy is consistently better than any of those in isolation. The fascia work creates the mobility window; the exercise rehab teaches the body to use it. Skipping the exercise side is one of the most common reasons people see only short-lived results from bodywork.
Evidence base — what research actually shows
Honesty matters here, because the marketing around fascia work is louder than the evidence behind it. A grounded read of the current literature:
Pain reduction. Moderate, replicated effect sizes for chronic low back pain, plantar fasciitis, and myofascial pain syndrome. The effect is meaningful — comparable to other manual therapies — but it is not a miracle. Patients who pair manual work with exercise show better outcomes than either alone.
Range of motion. Consistent short-term improvements in flexibility and joint range. The duration of the benefit depends heavily on whether the patient does follow-up movement work. Without it, gains often regress within days.
Post-operative recovery. Scar tissue mobilization is supported in specific contexts — abdominal surgery, c-section, mastectomy, joint replacement. Quality of evidence varies by surgery type. The pattern is consistent enough that most surgical rehab programs now include some form of scar mobilization.
Athletic performance. Honestly, limited high-quality evidence of direct performance gains. The strongest case is for recovery and injury prevention, not for making athletes faster or stronger.
Postural change. Short-term improvements are well-documented; durable structural change requires combining manual work with corrective exercise over months, not single sessions.
The honest summary: fascia work has real effects on pain and mobility, especially for chronic dysfunction, and especially when combined with exercise. The exotic claims (organ detox, emotional release, structural reorganization of the body) outrun the evidence. The conservative claims (this can help you move better and hurt less) are well-supported.
Cost and access — US versus Taiwan
Quality fascia work in the United States runs $80-150 per session in most markets, with specialty providers (oncology massage, prenatal-trained therapists, structural integration practitioners) charging more. Insurance rarely covers it.
In Taiwan, comparable sessions run $30-60 USD. The same level of training, often delivered by practitioners working in established clinics or wellness centers, at less than half the price. For chronic dysfunction that genuinely needs 6-12 sessions to resolve, the math changes — what costs $1,000+ in the US can be done for $300-500 in Taiwan, with the side benefit of a rest layer to the trip.
This is part of why so many people pair fascia work with a medical or screening trip to Taiwan. The economics let you actually complete a treatment arc instead of doing 2-3 sessions and stopping. For a fuller picture of how Taiwan fits into a wellness travel plan, see our guides to Taiwan as a fascia bodywork destination and why Americans find true wellness recovery in Taiwan.
What to expect — realistic timelines
For chronic dysfunction, plan on 3-6 sessions before judging whether fascia work is helping you specifically. Some people feel meaningful change after a single session — particularly for acute restrictions, headaches, or new-onset pain. Most people feel modest improvement after one session and noticeable change after three or four.
If you have done six well-executed sessions, paired with the home exercise work, and seen no change at all, the underlying problem is probably not fascial. That is useful information — it means it is time to revisit the diagnosis with a physician, physical therapist, or orthopedist.
If you are considering whether fascia work is worth trying for your situation, our services overview covers what is available, and the providers page lists practitioners and clinics with the training to do this well.
Sources & Further Reading
FAQ
For most people with chronic low back pain that has lasted more than three months, fascia work targeting the thoracolumbar fascia, glute medius, and hip flexors produces meaningful relief. Plan on weekly sessions for 4-6 weeks, paired with basic core and hip-extension exercises. If there is no improvement by session 6, the underlying cause may not be fascial — revisit the diagnosis with a physician or physical therapist.
Wait until your OB or surgeon confirms the wound is fully healed, typically 6-8 weeks for an uncomplicated c-section. Once cleared, gentle scar mobilization can reduce pulling sensations, improve abdominal function, and help with the low back pain that often follows c-section recovery. Look for a practitioner with prenatal or postpartum bodywork training.
After, or well in advance — not same-day. Same-day or pre-event fascia work can affect proprioception and tendon stiffness in ways that don't help performance. Schedule fascia work 2-4 days before a key event, or in the recovery window 24-72 hours after. Regular sessions every 2-3 weeks during training blocks support recovery without interfering with adaptation.
Monthly maintenance is enough for most office workers without active symptoms. If you have tech neck, headaches, or noticeable forward head posture, start with weekly sessions for 4 weeks, then taper to monthly. Pair the manual work with deep neck flexor exercises, scapular retraction drills, and hip flexor stretching — the bodywork creates the mobility window; the exercises lock in the change.
Yes — plantar fasciitis is one of the clearest indications for fascia work. The protocol works the foot itself, then the calves (gastrocnemius and soleus), then often the hamstrings, since the entire posterior chain pulls on the plantar fascia. Single-session relief is common; durable change usually takes 4-6 sessions plus eccentric calf loading at home.
Yes, with a practitioner trained in prenatal bodywork. The work should be gentle, side-lying after the first trimester, and focused on relief rather than deep restructuring. Hormonal changes (relaxin) already increase joint laxity, so aggressive techniques are inappropriate. Skip deep abdominal work entirely. Always check with your OB or midwife before starting any new bodywork during pregnancy.
Yes. Avoid fascia work if you have a suspected or confirmed deep vein thrombosis (absolute contraindication), an acute injury still in the inflammatory phase, recent surgery under 6 weeks, an active infection, severe osteoporosis without medical clearance, recent chemotherapy without oncology-trained practitioner, or open wounds in the area. Bleeding disorders and anticoagulant therapy require modified, lighter techniques rather than complete avoidance.